Traditional & Innovative Treatments For Strokes


Medical treatments save lives. Stroke victims who seek immediate treatment have the best chance to survive and eventually recover. But non-fatal strokes often have long-term debilitating consequences. Patients may require extensive therapy from skilled occupational therapists to reclaim their ability to speak, be mobile, and simply function in their daily lives.
As medicine evolves, innovative new treatments may prevent long-term stroke damage for many patients. Some new treatments work in coordination with existing medical treatments to make full recovery more likely. With these and traditional options, occupational therapists can have more favorable outcomes as they aid in stroke patients' recoveries.
A Look at the Various Treatments for Stroke Clots
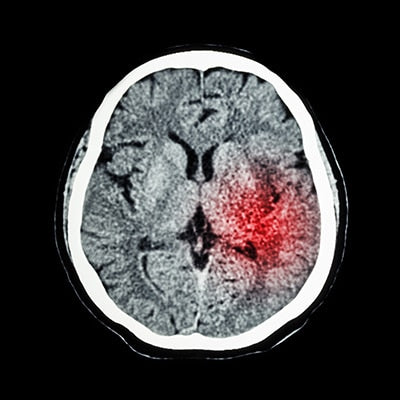
What is a Stroke?
During a stroke, a blood vessel is either blocked or it ruptures. This stops the brain from receiving the necessary blood flow and oxygen. Brain cells die and, as a result, the victim may suffer loss of coordination or brain function.
As medical science advances, we learn more about the brain and strokes. This increased knowledge and insight leads to new treatment options and improvements to existing procedures.
Any occupational therapist knows that recovery from a stroke is rarely easy. However, innovative treatment methods relieve pain, help patients recover brain function, and empower patients to lead full lives.
The best treatment option depends on the kind of stroke and finding the right occupational therapist. According to the American Stroke Association, there are two different types of stroke: ischemic or hemorrhagic. Since prompt medical attention greatly improves the chance of recovery, if you or anyone you know may be suffering from a stroke, it is crucial that you seek immediate medical care.
Ischemic Stroke Treatment Options
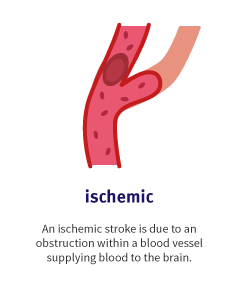
An ischemic stroke is due to an obstruction within a blood vessel supplying blood to the brain. This is the most frequent type of stroke as it accounts for about 87 percent of all stroke cases.
Tissue Plasminogen Activator Treatment
A common and only FDA-approved treatment for ischemic strokes is tissue plasminogen activator treatment (tPA), which is delivered through an IV in the arm.
A tPA treatment dissolves the clot to improve blood flow to the affected part of the brain. An intravenous injection of tPA is very effective for smaller blood clots; however, it often fails to break up larger clots.
A tPA treatment should happen within the first 3 hours after detecting symptoms, though it is effective for some patients within 4.5 hours. Unfortunately, many stroke sufferers don’t seek treatment soon enough. This is why immediate treatment is crucial.
Mechanical Thrombectomy and Stent Retriever Therapy
Previously, tPA was the only FDA-approved treatment for acute stroke. However, multiple trials indicate that a new treatment is effective for many patients; a mechanical thrombectomy is a breakthrough treatment involving a stent.
A stent is a tiny wire-mesh tube that props open an artery. The stent is inserted into the body. It opens and captures the clot so doctors can remove the stent along with the trapped clot.
Stent retriever therapy is a new procedure experts call the most major advance in stroke treatment in two decades.
A mechanical thrombectomy procedure should be done within six hours of acute stroke symptoms and also only after a patient receives tPA. Time is still of the essence—91% of patients who receive the treatment within 2.5 hours avoid permanent disability.
Detachable Coil Technique
Another promising new therapy is detachable coil technique, which is a new treatment of high-risk intracranial aneurysms. The treatment involves inserting a small platinum coil into an artery in the thigh. It is then threaded through the arteries and to the aneurysm. The surgeon releases the coil into the aneurysm.
The goal is to evoke an immune response from the body. The body produces a blood clot within the aneurysm. This clot strengthens the artery walls and reduces the risk of rupture. Once stabilized, a neurosurgeon clips the aneurysm with less risk to the patient.
Carotid Endarterectomy
Another common treatment for blocked arteries is carotid endarterectomy. Carotid endarterectomy is a surgical procedure that removes plaque from the arteries that run along each side of the neck. The surgeon makes an incision to open the carotid artery and then removes plaque causing the blockage. Then the surgeon repairs the artery with stitches or graft. The procedure may reduce your risk of future ischemic stroke, but it also involves risks for people with heart disease or other medical conditions.
Angioplasty and Stents
Like carotid endarterectomy, angioplasty can also work to open the arteries again. Angioplasty is a treatment where a surgeon gains access to your carotid arteries and inserts a balloon to expand the artery. This is typically done through an artery in the groin. The surgeon navigates to the carotid arteries in the neck. After the balloon expands the narrowed artery, a stent can be inserted to support the opened artery.
Hemorrhagic Stroke Treatment Options
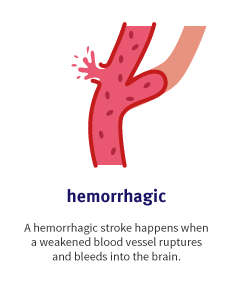
A hemorrhagic stroke happens when a weakened blood vessel ruptures and bleeds into the brain. This potentially fatal outcome most commonly results from high blood pressure. A hemorrhagic stroke accounts for 20 percent of all strokes, according to the American Stroke Association.
Normally, in a healthy brain, neurons and blood do not come into direct contact. Instead, necessary oxygen and nutrients travel across a blood-brain barrier to the neurons. The glia, or nervous system cells that protect neurons, create this blood-brain barrier. The barrier surrounds blood vessels and capillaries, controlling which parts of the blood can pass through. During a hemorrhagic stroke, an artery in the brain bursts, blood spews out into the surrounding tissue and upsets not only the blood supply but the delicate chemical balance neurons require to function.
Surgical AVM Removal
Surgical AVM removal can be done to remove the blood vessel before it ruptures to prevent a stroke from happening. An AVM or Brain Arteriovenous Malformations is composed of an abnormal collection of blood vessels with weakened walls. A surgeon can remove a smaller AVM when it is detected if it is in an accessible location of the brain. The intention is to eliminate the risk of rupture and protect against bleeding from the AVM in the future.
Endovascular Procedures
Surgical procedures are frequently used to treat hemorrhagic strokes, but some times less invasive endovascular treatments are sufficient. A physician inserts a catheter, introduced through a major artery in the leg or arm. The catheter is then guided to the aneurysm or AVM and is used to deposit a mechanical agent, like a coil, to prevent further rupture.
Common Surgical Treatments for Hemorrhagic Stroke
Depending on the situation, numerous surgical procedures are used to treat hemorrhagic strokes. Here is a brief overview of a few options:
- Clipping is where a surgeon places a tiny clamp at the base of the aneurysm. This stops blood flow to it and prevents bursting or further bleeding.
- Coiling (endovascular embolization) is when a surgeon inserts a catheter into an artery and guides it to the brain using X-ray imaging. Next, the surgeon guides detachable coils into the aneurysm to block blood flow so the blood clots.
- The intracranial bypass treatment can be used in unique circumstances to help treat poor cerebral blood flow.
- Stereotactic radiosurgery is a procedure involving multiple beams of highly focused radiation. The beams are used to repair vascular malformations in this advanced, less invasive treatment.
Stem Cell Treatment
Stem Cell Treatment is a promising new development for stroke treatment. Stanford University School of Medicine investigators conducted a small trial that indicated that stem cell treatment appears both safe and effective in restoring motor function in chronic stroke patients.
Researchers injected modified, adult human stem cells directly into the patients’ brains. Patients saw improvement in motor function without dangerous side effects. Due to the promising results, an expanded trial is now in the works.
According to Dr. Gary Steinberg, professor and chair of neurosurgery at Stanford, “It was designed primarily to test the procedure’s safety. But patients improved by several standard measures, and their improvement was not only statistically significant but clinically meaningful. Their ability to move around has recovered visibly. That’s unprecedented. At six months out from a stroke, you don’t expect to see any further recovery.”
Stroke patients showed significant recovery by a number of measures within a month’s time after the stem cell treatment was done, and they continued improving for several months afterward, anywhere from 6 and 12 months after surgery.
Medical Progress
As medical science progresses, these new treatments offer better recovery from strokes with potentially fewer side effects than traditional ones. Older treatments still save lives and provide relief from further complications, but some new treatments may expand the number of patients who benefit from acute stroke treatment. For both older and emerging treatments, patients who seek immediate medical care typically have the best chance of recovery.
All content provided on this blog is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you think you may have a medical emergency, call your doctor or 911 immediately. Reliance on any information provided by the Saebo website is solely at your own risk.
All content provided on this blog is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition. If you think you may have a medical emergency, call your doctor or 911 immediately. Reliance on any information provided by the Saebo website is solely at your own risk.



