
Regaining Shoulder Function After Stroke: Common Clinical Concerns & Strategies

When blood flow to certain regions of the brain is cut off from a stroke, that particular communication center no longer relays messages to corresponding parts of the body. So, as with all stroke issues, the problem begins in the brain but becomes aggravated by the weakening of the body part itself. The key to rehabilitation is focusing on understanding both the mind’s neuroplasticity and the body’s physical strengthening.
The shoulder is a complex and well-balanced system of joints, ligaments, and bones. When these parts work together in harmony, the shoulder acts as the primary guide for the arm and hand. If a stroke occurs, any disruption to this system may set off a series of complications throughout the upper body and impede with everyday activities. Understanding the shoulder's system is crucial to resuming daily activities after a stroke. While healing the shoulder may feel daunting, it’s important to remember that there are many rehabilitation options out there.
During the rehabilitation process, stroke survivors often experience shoulder complications including stiffness, spasticity, flaccidity, or pain. It is important to thoroughly examine the shoulder if these complications arise after a stroke to determine the best course of treatment.
[optin-monster-shortcode id="bvwkd4t2a1fqpkndqvqa"]Common Shoulder Concerns After Stroke
Along with impeded mobility, one of the first issues stroke survivors will have to grapple with is increased pain and discomfort. A quality rehabilitation plan should address individual issues as they arise, but it’s important that stroke survivors, caregivers, and loved ones understand the root causes & treatments of shoulder issues.
Many stroke survivors deal with hemiparesis, the weakness of one side of the body, which often leads to shoulder issues. Specific concerns may include:
- Subluxation: a partial dislocation of the shoulder when the muscles in the area weaken and do not hold the shoulder in place.
- Spasticity: the neuromuscular condition usually caused by damage to the portion of the brain or spinal cord that controls voluntary movement.
- Frozen shoulder: a condition where the tissue that surrounds the shoulder thickens and creates scar tissue, and also produces less fluid which limits lubrication. As a result, shoulder movement is limited and painful.
- Impingement: a condition where the rotator cuff tendons are intermittently trapped and compressed during shoulder movements, causing injury to the shoulder tendons and bursa which results in painful shoulder movements.
With such a highly connected region of the body, early intervention is crucial, as one symptom can strongly affect another, leading to further weakness and pain.

Subluxation in Stroke Survivors and Treatment
A strong shoulder requires a healthy system of interconnected parts, including the shoulder bones, muscles, and joint capsules. If one area is disrupted, the rest of the system becomes imbalanced.
Subluxation occurs when the bone in the upper portion of the arm—or humerus bone—is dislocated from the shoulder socket. The shoulder blade—or scapula—then adjusts to the surrounding muscles, altering the natural state of the area.
Complications, such as weakness or spasticity, in either area may lead to post-stroke shoulder displacement or subluxation. Both symptoms are quite common in the affected limb or another area of the body. In the time just after the stroke, a weak or paralyzed arm often hangs down at the side of the body, subjecting the arm to the effects of gravity and stretching tissues to the point of dislocation. Without the support of the shoulder muscles, the joint capsule stretches causing subluxation. Spastic muscles can also cause joints to become displaced.
The most important factor in preventing subluxation is keeping the arm and shoulder in a properly supported position. This protects the joint from the damaging gravitational pull that can strain the ligaments. Otherwise, the threat of subluxation increases. Subluxation slings can often be helpful as part of a broader treatment regimen to support the arm and minimize pain. However, research does not support slings alone as a way to improve or reduce subluxation.
Stroke survivors may also find success treating subluxation with electrical stimulation, which sends electrical impulses to the weakened muscles (proximal migrators) to stimulate a contraction causing the humerus to migrate upward. Some of the benefits survivors may experience from electrical stimulation include decreased pain, increased circulation, decreased inflammation and improved overall function.
Frozen Shoulder in Stroke Survivors
Often difficult to understand, frozen shoulder involves the contracture and thickening of the fibrous capsule around the ball-and-socket joint of the shoulder. It is also often referred to as immobilization arthritis, adhesive capsulitis, or stiff shoulder. Understandably, this combination of fibrosis and inflammation causes pain therefore decreasing range-of-motion in the shoulder. Doctors find that up to 25% of stroke survivors experience some form of frozen shoulder in the first six months. Additionally, nearly three-quarters of those with hemiplegic shoulder pain often receive the diagnosis.
Three Stages Of Frozen Shoulder
In 1975, B. Reeves determined three common stages of frozen shoulder. These involve the cycle of pain, stiffness, and recovery:
Stage 1: Freezing Stage of Frozen Shoulders. The more painful stage; stiffness and soreness develop over a period of 2-9 months. This growing pain restricts the range of motion and decreases coordination in the arm and shoulder.
Stage 2: Frozen Stage of Frozen Shoulders. Marked by significant stiffness, the frozen stage can last between four months and a year. This is when doctors believe the fibrous capsule thickens and adheres to the humeral head.
Stage 3: Thawing Stage of Frozen Shoulders. Once the adherence is complete, those experiencing frozen shoulder will slowly regain range of motion over a period of five to twenty-six months.
Frozen Shoulder Treatment Options for Stroke Survivors
Treatment for frozen shoulder, or fibrosis of the shoulder joint, all comes down to controlling inflammation and keeping the joint in motion. Over-the-counter Nonsteroidal Anti-Inflammatory Drugs (NSAIDS) such as ibuprofen and aspirin, relieve pain-causing inflammation that restricts full range of motion. Once the person undergoing rehab is able to move more freely, stretching exercises work the shoulder out of the frozen position.

Impingement in Stroke Survivors
Shoulder impingement syndrome is a condition where your shoulder rotator cuff tendons are intermittently trapped and compressed during shoulder movements This causes injury to the shoulder tendons and bursa resulting in painful shoulder movements. The symptoms are typically a limited range of motion, as it relates to reaching upwards behind the back, along with shoulder weakness and pain during overhead use of arm.
Impingement can be addressed through anti-inflammatory medications coupled with a stretching regimen that gently strengthens the affected muscles and stretches the soft tissue that is shortened. A routine like this is best developed with the care and guidance of professionals, as anti-inflammatory medications can be harmful when taken long-term and exercises should be thoughtfully structured so they do not cause further pain or injury.
Spasticity in Stroke Survivors
Spasticity is a neuromuscular condition typically evidenced by involuntary muscular contractions or movements. On the milder end of the spectrum, stroke survivors who experience spasticity may experience tightness or stiffness in the affected muscle area. More severe cases of spasticity can involve painful and uncontrollable spasms.
There are various treatment options for spasticity. A primary one is the use of oral medications, such as Baclofen or Botox, to directly address spastic muscles or stiffness. They work best in combination with stretching exercises, existing as part of a routine meant to regain range-of-motion and muscle strength and agility. The SaeboStretch or SaeboFlex can also be helpful tools in addressing spasticity, depending on the severity of the case.
Products That Can Transform Your Shoulder Rehab

Luckily for stroke survivors and their families, there are a variety of devices on the market that can help assist the weak shoulder to allow it to engage in necessary exercises and activities. For example, the SaeboMAS is a zero-gravity arm support that would be an ideal assistive device for many individuals with moderate to severe shoulder weakness. Additionally, the SaeboMAS mini is a smaller version that is perfect for home therapy and pediatric rehabilitation. The SaeboGlide is another option, specifically designed to constructively challenge stroke survivors at all stages of recovery. By using a gliding sleeve, stroke survivors can perform various controlled arm exercises at an appropriate strength level.
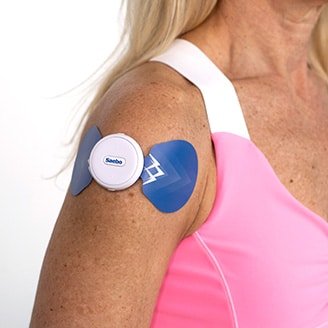
If electrical stimulation is part of a stroke survivor’s rehabilitation program, the SaeboStim One, a wireless electrical stimulation device, is designed to prevent or reduce muscle weakness by strengthening the affected muscles. The affordable and compact device works by delivering electrical signals through its wireless electrodes to the targeted affected muscle groups. The SaeboStim One's program parameters are clinically designed to slow down weakness and strengthen impaired muscles.
Learn more about Saebo products from Saebo patients and Saebo-trained Occupational Therapists on our testimonials page.
Shoulder Exercises for Stroke Survivors

While these assistive devices are helpful for stroke survivors working to recover shoulder function, there are also a variety of shoulder rehabilitation exercises that can be done from home.
Basic-Level Shoulder Exercises

Towel Slide (Basic)
Spread a towel on a desk or table and sit or stand in front of it. Lay the affected arm flat on the towel with your unaffected hand directly on top of it. With the help of your stronger arm, push the bottom hand and the towel away from you across the table. The body will naturally shift into a position that stretches the shoulders in a safe manner. Continue to move forward as far as possible and without causing pain, increasing the distance each time the exercise is completed.

Shoulder Shrug
With the use of a mirror that shows your whole top half of the body, lift your stronger shoulder up to the side of the head in a slow shrugging motion. From this raised position, roll the shoulder back slowly, bringing the two shoulder blades closer together. Repeat this action a few times a day, realigning the shoulder blades as you go.
Intermediate-Level Shoulder Exercises

Towel Slide (Intermediate)
Similar to the basic-level shoulder slide, lay the towel on a table before you and place your affected hand below the stronger one. Slide the arm forward as before, but use this position to also explore a side-to-side motion. The goal is to eventually work up to include a circular, forward, and side-to-side motion.

External Rotation With Cane
With a lightweight cane or umbrella, grasp it in front of you with both hands and bend the arms at a 90-degree angle by the elbows. Begin by moving the cane out to one side, keeping forearms as straight as possible, without letting them fall. Then move to the other side and repeat as necessary.
Advanced Shoulder Exercises

Behind-the-Neck Cup Pass
Choose several stackable cups and place them in front of you on a table. Focus your vision ahead of you, not on the cups, then delicately pick up the top cup and pass it behind your neck, using your opposite hand to receive the cup and place it back on the table. Continue this exercise until the stack is complete.

Behind-the-Waist Cup Pass
As before, stand or sit before the stack of cups. This time, pass each cup from hand to hand, but circle behind the waist instead of the neck. This exercise strengthens different muscles in the arms while increasing the range of motion.
Shoulder Complications During Stroke Recovery Can Be Overcome
The majority of strokes occur in people older than 65, but risk begins to increase after the age of 55. Survivors of any age can take action to improve their quality of life, so it’s important to remain hopeful and proactive. If you’ve suffered a stroke and have lost mobility as a result, employing a combination of exercises, assistive devices, and expert recommendations should help get you started in the process of reclaiming control and retraining your joints and muscles.
All content provided on this blog is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you think you may have a medical emergency, call your doctor or 911 immediately. Reliance on any information provided by the Saebo website is solely at your own risk.
All content provided on this blog is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition. If you think you may have a medical emergency, call your doctor or 911 immediately. Reliance on any information provided by the Saebo website is solely at your own risk.



